What is psoriasis?
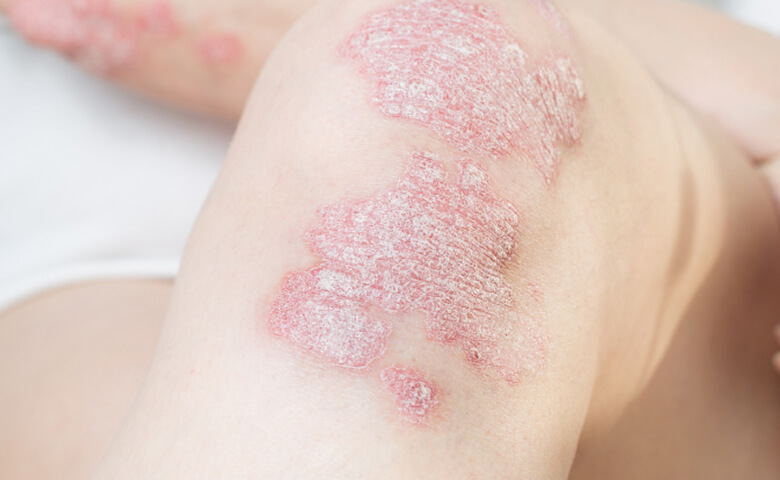
Psoriasis is a long-term inflammatory skin condition that causes red, scaly plaques on the skin. These plaques can itch, crack, sting, or feel tight, and they often come and go without much warning. For many people, psoriasis is more than a visible rash. It can affect sleep, clothing choices, work, relationships, and confidence.
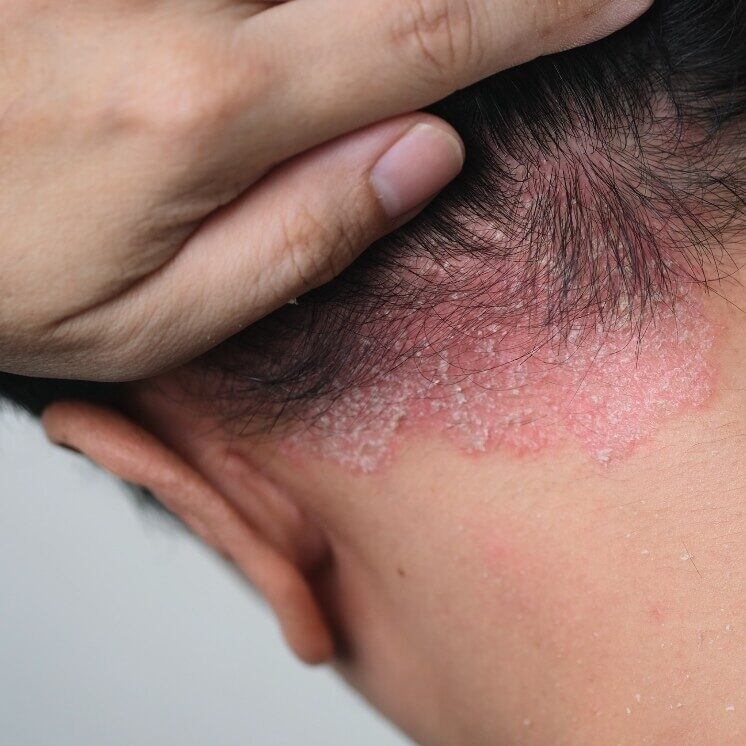
A key feature of psoriasis is the rapid buildup of skin cells, which leads to thick scaling. Commonly affected areas include the scalp, elbows, knees and lower back, although psoriasis can appear anywhere. Scalp psoriasis is particularly common and can be difficult to manage without the right treatment approach.
Psoriasis can also affect:
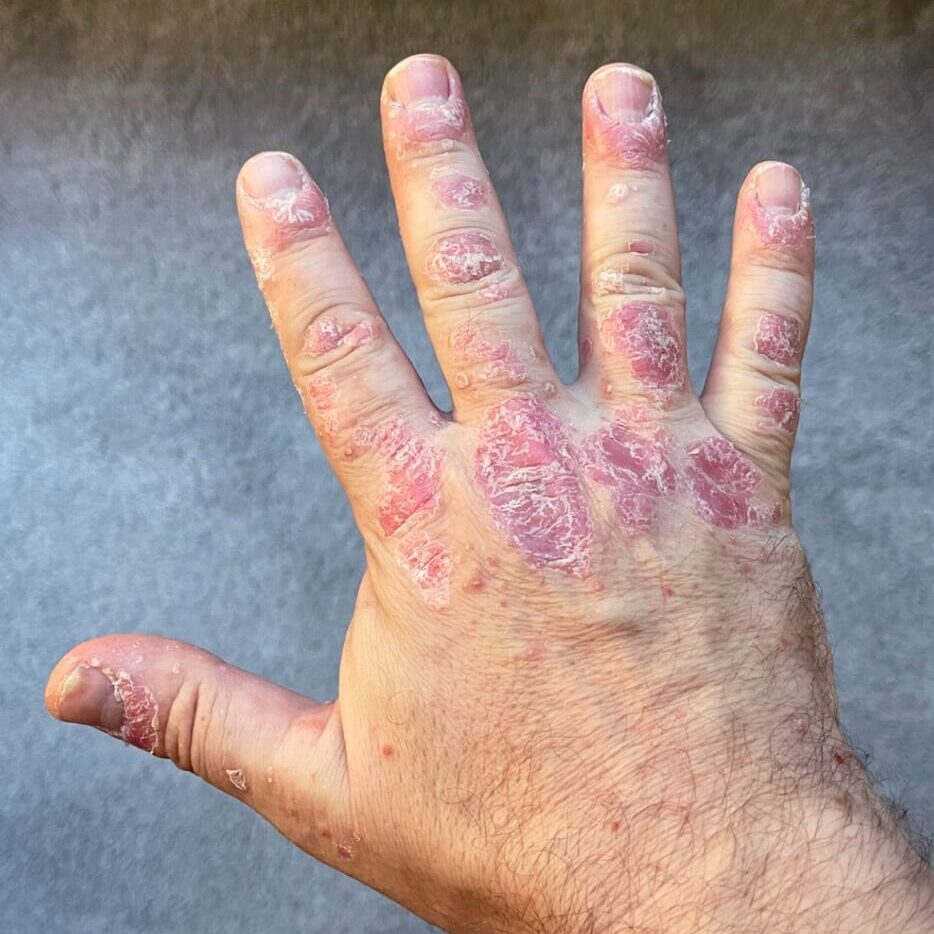
- The palms and soles, where thick scale may split and become painful
- The nails, causing thickening, lifting from the nail bed, or a rough, pitted surface
- The genitals and groin, armpits and under the breasts, where the skin may become red but without the thick scale
In some cases, psoriasis is linked to joint inflammation known as psoriatic arthritis. This can cause pain and swelling in the fingers, toes, or lower back and may interfere with movement, work, and everyday tasks.
If your symptoms are persistent or interfering with daily life, speaking with a psoriasis dermatologist online can help you get clarity on what type of psoriasis you have and what treatment is most likely to settle it.
Who gets psoriasis?
Psoriasis affects around 2 to 4 percent of the population and occurs across all ages, genders, and ethnic backgrounds. While it can begin at any stage of life, it often first appears between the ages of 20 and 40.
UV light can improve psoriasis for some people, which may explain why it is less common in sunnier climates. Even so, most people require medical treatment to properly control psoriasis, particularly when symptoms involve the scalp, nails, joints, or larger areas of skin.
What causes Psoriasis?
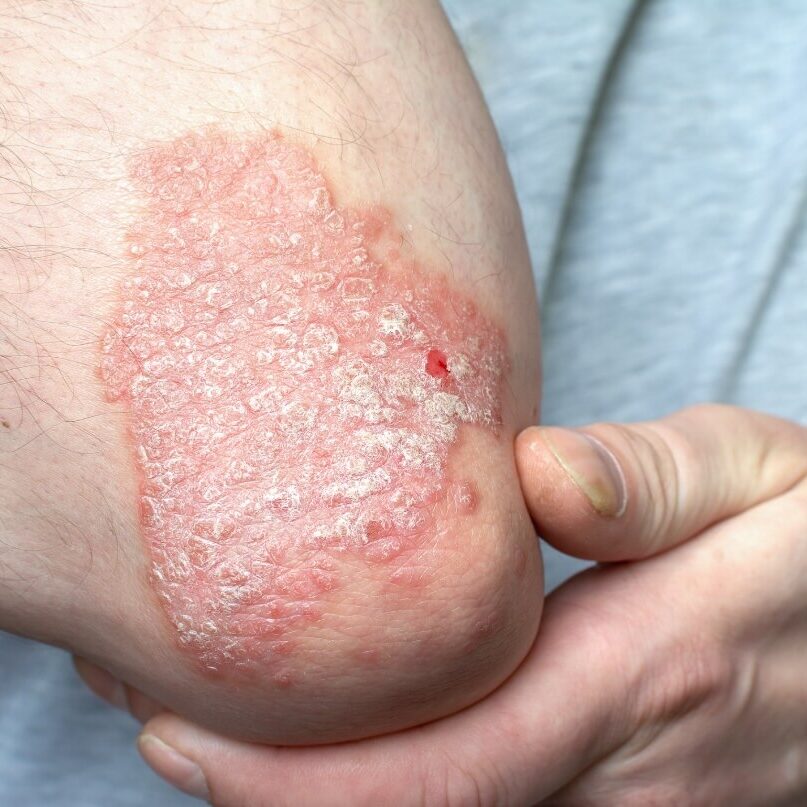
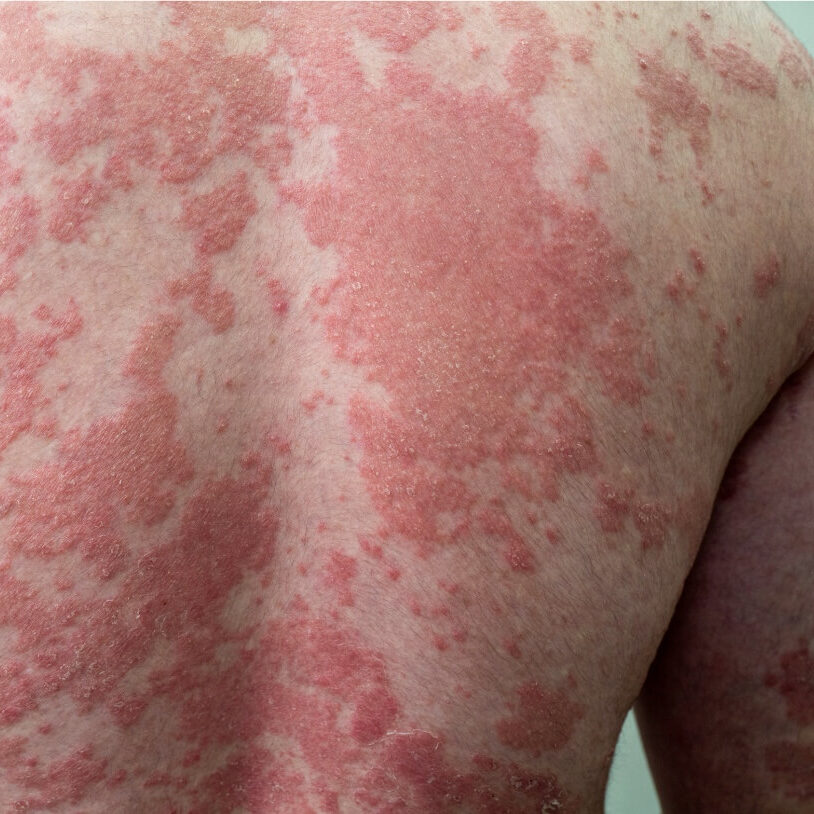
Psoriasis is caused by an overactive immune response in the skin. Certain immune cells mistakenly become active in the upper layers of the skin, leading to inflammation, redness, and scaling, despite there being no infection.
The condition develops due to a combination of genetic factors, immune system changes, and environmental triggers. Psoriasis is also associated with inflammation elsewhere in the body, which explains why it can be linked with joint disease and other health conditions.
Genetics
Psoriasis is not caused by a single gene. People with psoriasis have different combinations of genes that increase their susceptibility. While psoriasis can run in families, this occurs in only a portion of cases.
Immune system changes
People with psoriasis do not have a weak immune system. Instead, a specific part of the immune system is overactive, driving inflammation in the skin and sometimes the joints.
Triggers and lifestyle factors
In people who are predisposed, psoriasis may be triggered or worsened by external factors. Stress is one of the most common triggers. Infections such as streptococcal throat infections can cause sudden flare-ups, particularly guttate psoriasis. New plaques may also appear at sites of skin injury.
Certain lifestyle factors can worsen psoriasis symptoms:
- Smoking, particularly in palm and sole psoriasis
- Excess weight, which increases inflammation
- Alcohol, which can aggravate symptoms in some people
Identifying and managing triggers is an important part of how to treat psoriasis and reduce flare frequency.
Your Psoriasis treatment options
Psoriasis treatment depends on the type of psoriasis, the areas involved, and how much the condition affects your quality of life. The goal is to reduce psoriasis symptoms, clear plaques as much as possible, and prevent flare-ups from disrupting daily life.
General measures
These steps can support medical treatment:
- Stopping smoking
- Limiting alcohol intake
- Managing stress
- Maintaining a healthy weight and regular exercise
Topical treatment
Often used for mild to moderate psoriasis, or alongside other treatments:
- Corticosteroids with or without calcipotriol (a form of Vitamin D)
- Compounded creams containing salicylic acid, tar, or dithranol
- Tar shampoos for scalp psoriasis acid, tar, or dithranol
- Tar shampoos for scalp involvement
UV phototherapy
Phototherapy uses a controlled form of UVB light delivered in dermatology clinics:
- Usually required 2 to 3 times per week for at least 20 sessions
- Aims to clear the skin, then reduce treatment frequency to lower relapse risk, then to consider a lower dose or frequency to reduce the chance of psoriasis returning
Oral medications
These treatments work on the immune system to reduce inflammation:
- Methotrexate
- Ciclosporin
- Apremilast
- Deucravacitinib
Acitretin, a medicine derived from vitamin A, reduces the thick scaliness of psoriasis plaques.
Injectable medications (biologics)
Biologic treatments target specific immune pathways involved in psoriasis. They are injected under the skin every 1 to 3 months and are often used for moderate to severe psoriasis or when other treatments have not worked. These medicines can also help manage psoriatic arthritis.
An online dermatologist can assess whether these treatments are appropriate for your symptoms and guide ongoing care.
What can your Psoriasis treatment outcome look like?
Psoriasis can be mild, moderate, or severe, and outcomes vary from person to person. Earlier onset and more extensive disease are more likely to persist long term, while milder psoriasis may come and go.
With current psoriasis treatment options, many people can achieve clear or almost clear skin and maintain that improvement for long periods. For patients, this often means:
- Less itch, soreness, and scaling
- Fewer visible plaques on the scalp and body
- Better sleep
- Less disruption to work, exercise, and social life
- Improved confidence and comfort day to day
Flare-ups can still occur, but having a clear treatment plan reduces how often they happen and how much they affect your life. There is also growing evidence that earlier treatment can improve the course of your psoriasis severity in future.
If psoriasis is affecting your wellbeing, booking an online appointment allows you to speak directly with an experienced dermatologist without attending a clinic. Digital Dermatology also manages a wide range of other skin conditions through our online dermatology services, so care can continue even if your concerns extend beyond psoriasis.
For an understanding of how online dermatology pricing compares with attending a clinic in person, including consultation structure and follow-up, see our consultation fees.